
Dr. J. W. "Skip" Truitt jr.
The past decade has seen orthopedic and orthodontic therapy assume their justified status in general dentistry along side that of emplantology, endodontics and reconstruction. And as in all areas of dentistry there is a great debate as to which treatment philosophy is best. Unfortunately many of us become so involved as to which orthopedic appliance to select or what precise angulation to choose in a bracket system that we frequently lose sight of our overall treatment objectives.
Having lectured worldwide for the better part of twenty years, I am constantly amazed at how often we as a profession must rediscover the wheel. For example, when one reads the current orthodontic journals it appears that arch development and mandibular repositioning are a newly discovered state of the art concept, and obviously nothing could be further from reality. It is equally amazing that different treatment philosophies can view the same malocclusion, prescribe a very precise treatment regime, and still not comprehend the basic underlying problems that are involved in the first place. This lack of understanding frequently results in less than satisfactory therapy.
It is my opinion that correct diagnosis and treatment planning should center around four basic principles. Once these principles are well understood then the actual appliance system used to obtain these objectives becomes a matter of personal choice for the individual practitioner. I would like to list these four principles for you, and then examine each one separately and discuss how different treatment philosophies attempt to obtain these objectives.
Let's begin first by discussing the concept that all cases treat to the mandibular arch. Angles, was the first to document in literature the importance of the Class I relationship of the maxillary first molar to the mandibular first molar. Unfortunately, he did not fully appreciate the influence of a skeletal imbalance upon this molar relationship nor the technical problems involved in precisely positioning the teeth. In addition, he assumed that this Class I relationship could always be obtained on a non-extraction basis. However, he did understand the critical importance of balancing the maxillary dentition to the mandibular base.
Next on the scene was the concept of extracting teeth, usually the first bicuspids, to obtain this Class I balance. When reviewing the literature for cases treated with first bicuspid extraction therapy, one must turn to Tweed and Begg for standards in treatment philosophy. Both techniques produced highly successful results when applied to skeletal Class I cases where the malocclusion was caused by either arch length loss or macrodontia. When these techniques were applied to skeletal Class II, skeletal Class III or constricted arch cases the failure rate increased dramatically.
The questions must then be asked that if the underlying cause of malocclusion is skeletal, can it be treated by extraction or non-extraction orthodontic therapy only? While the obvious answer to this question is no, it is not a definite no. It is possible to obtain dental alveolar base compensations for skeletal imbalances as long as these imbalances are very moderate in nature. The greater the skeletal imbalances the more compensation compromises the overall therapy.
The importance of orthopedic correction for skeletal malocclusions has been addressed for decades by Schwarz, Crozat, Bimler and Balters to name only a few. Therefore, when one makes a correct diagnosis between a dental and skeletal malocclusion, understand the appliance systems involved to correct these malocclusions, and realizes that the entire case is to be treated to the lower arch, then therapy becomes relatively straight forward.
For example, it is impossible to obtain the correct size and position of the mandible to the anterior cranial base until the maxilla is properly developed in size and position to the anterior cranial base first. In my hands the maxillary three directional appliance is best suited for developing the size of the maxilla and the reverse pull head gear, or face mask as it is sometimes called, is best to treat a maxilla that is retrognathic to the anterior cranial base.
While the maxilla is being developed in size and/or position the size of the alveolar ridge on the mandibular base can be increased. The correct sequence of development is as follows:
(1) The maxillary sagittal correction is always one month ahead of the maxillary transverse correction.
(2) The maxillary transverse correction is always one month ahead of the mandibular transverse correction.
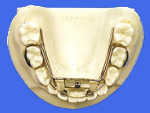
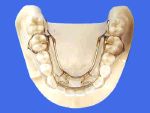
Many times the mandibular arch is not only underdeveloped in size, but it has also suffered some degree of arch length loss. It is this loss of lower arch length that forces many clinicians to resort to extraction of either first bicuspids or second molars. Appliances such as the Williams in the mixed dentition (fig. 1) and the Crozat in the permanent dentition (fig. 2) not only increase the lower arch size, but they also regain lost lower arch length.
Their mechanical advantage lies in the use of a body wire as opposed to an expansion screw for their active force. Therefore, these appliances are usually more effective in treating the lower arch than a Schwarz appliance or the mandibular portion of the Clark Twin Block TM which creates only a change in transverse arch size.
Once the maxilla has been properly developed in size and correctly positioned, and the alveolar ridge on the mandible base has been correctly developed, the next step in the treatment sequence is to position the mandible into it's correct relationship with the maxilla and in turn to the anterior cranial base. Appliances such as the Bionator, the Clark Twin BlockTM, and the Rick-A-Nator can be utilized to obtain this mandibular repositioning.
At this point in the therapy we have created a skeletal Class I, and any remaining malocclusion is best correct ed with fixed appliance therapy on a non-extraction or extraction basis. The treatment objective is a Class I molar relationship as described by Angles and later refined by Andrews as being contact between and the distal buccal cusp of the maxillary first permanent molar and the mesial buccal cusp of the mandibular second permanent molar.
When treatment is complete the mandible is the correct size and is in it's proper relationship to the anterior cranial base; and all of the maxillary dentition is correctly related to the mandibular dentition.
Therefore, the entire case has been treated to the mandibular arch both dentally and skeletally. This brings us to the second of our four basic treatment principles. The critical area in the mandibular arch is the inter-canine width. This is probably the only treatment objective that is common to all orthodontic techniques and extends into their concepts of long term retention. For example, Rickett's technique for long term retention is to over rotate the mandibular cuspids and establish a locking effect of the inter canine area.
When the lower inter-canine width is incorrect there are only two treatment options open. One must either increase the inter-canine width by developing it, or extract teeth to compensate for the crowding of the lower anterior segment.
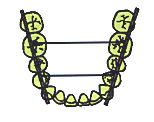
This presents the obvious question as to what is the correct lower inter-canine width? This is usually best determined by evaluating the overall size of the mandibular arch according to the Schwarz analysis. Once this is done the mandibular cuspids should fall on a straight line which passes over the buccal cusps of the bicuspids (on deciduous molars) and the mesial buccal cusp of the first permanent molar. (fig. #3)
There are a number of appliances width. These include the Jackson Crozat, Schwarz and Ker-Ant appliances. In most cases all lower anterior crowding can be corrected by properly developing the lower inter-canine width, and in the process recovering any lost mandibular arch length. However, if the lower inter-canine width is correct and the incisors are still crowded or excessively protrusive then extractions are definitely indicated. The two most common causes for this lower anterior malocclusion are macrodontia and severe mandibular arch length loss. These are problem both totally dental in nature and lend themselves quite well to extraction therapy.
Therefore all cases, even extraction cases, treat to the lower inter-canine width. At this point it is well worth discussing the negative effects of incorrect extraction therapy. The most classic error occurs when bicuspids are extracted to treat skeletal Class II. The treatment objectives in this situation are to eliminate lower anterior crowding and allow the mandibular molars to move forward into a more favorable Class I relationship, closing the remainder of the lower extraction site. The maxillary molars are either anchored or distal driven with extra oral traction to a Class I relationship, and the anterior overjet is eliminated by retracting the maxillary incisors into the upper extraction sites.
The net result of this approach is to leave the skeletal Class II problem untreated, and to correct the skeletal overjet dentally by retracting the maxillary incisors into an abnormally retrusive position. This in turn can create serious dysfunctions within the temporomandibular joints and produce very unaesthetic facial imbalances.
The point to be made is that dental units should not be extracted in an attempt to compensate skeletal horizontal or transverse imbalances. Extraction therapy is a rational approach to correcting a dental malocclusion only.
The third basic treatment principle is that only a Class III malocclusion is treated to the maxillary arch. The concept for Class III treatment is that the maxilla is the limiting factor for therapy. Once the maxilla has been fully developed in size to it's maximum genetic potential using an orthopedic appliance (usually a three directional appliance); and once the maxilla has been correctly positioned for ward to the anterior cranial base using a reverse pull head gear; the maxilla must be able to properly house or contain the mandible and maintain correct temporomandibular joint function. If the mandible cannot be then surgery must be performed to reduce the overall size of the mandible.
Class III fixed orthodontic therapy employs the same principle of treating the mandibular dentition to the maxillary dentition.
Therefore all Class III cases, including surgical cases, treat to the maxillary arch.
Fourth and probably most ignored of all treatment principles is the temporomandibular joints must function correctly in all cases. There is still the unfortunate misconception in many orthodontic techniques that temporomandibular joint dysfunction is totally unrelated to the patient's occlusion. In reality dental and skeletal malocclusions are the primary cause of most temporomandibular joint dysfunctions.
Malocclusions such as crossbites, a division two, and a unilateral skeletal Class II place tremendous dysfunctional forces on the temporomandibular joints. However even more destructive are orthodontic forces that cause a permanent distalising effect on the mandible, and in turn the mandibular condyles on their meniscus. The single most common mechanical mistake is over retraction of the maxillary incisors which is an inherent error if extraction therapy is preferred on the skeletal Class II patient.
So, irregardless of the malocclusion or the techniques being employed to treat it, the temporomandibular joints must be allowed to function correctly throughout the remainder of the patient's life.
The four basic treatment concepts are therefore very straight forward when viewed in proper perspective.
Once the clinician masters these basic concepts of therapy, the actual appliance systems that are selected are governed by the nature of the malocclusion and by the preference of the individual dentist.
I present a series of five highly concentrated seminars that allow the doctor and his or her staff to understand and obtain these goals. For additional information on the individual seminar contents and locations, or assistance in treatment planning and appliance selection and adjustments, please contact the Clinical Foundation of Orthopedics and Orthodontics.